Background
The human body functions through an intricate interplay of systems, and the interaction between the heart and brain stands out as one of the most remarkable connections1. The heart and brain, though anatomically distinct, are physiologically inseparable. Emerging evidence highlights that cardiovascular health profoundly influences brain integrity, cognitive function, and mental well-being2. Current systematic reviews collectively emphasized this interplay across structural, functional, and biochemical dimensions, underscoring the need for an integrated cardiovascular–neurocognitive perspective in clinical research and patient care. Therefore, this article brings forward some of the interesting scientific findings to illuminate the heart–brain connection, and address its compounding impact on an individual’s cognition and mental health.
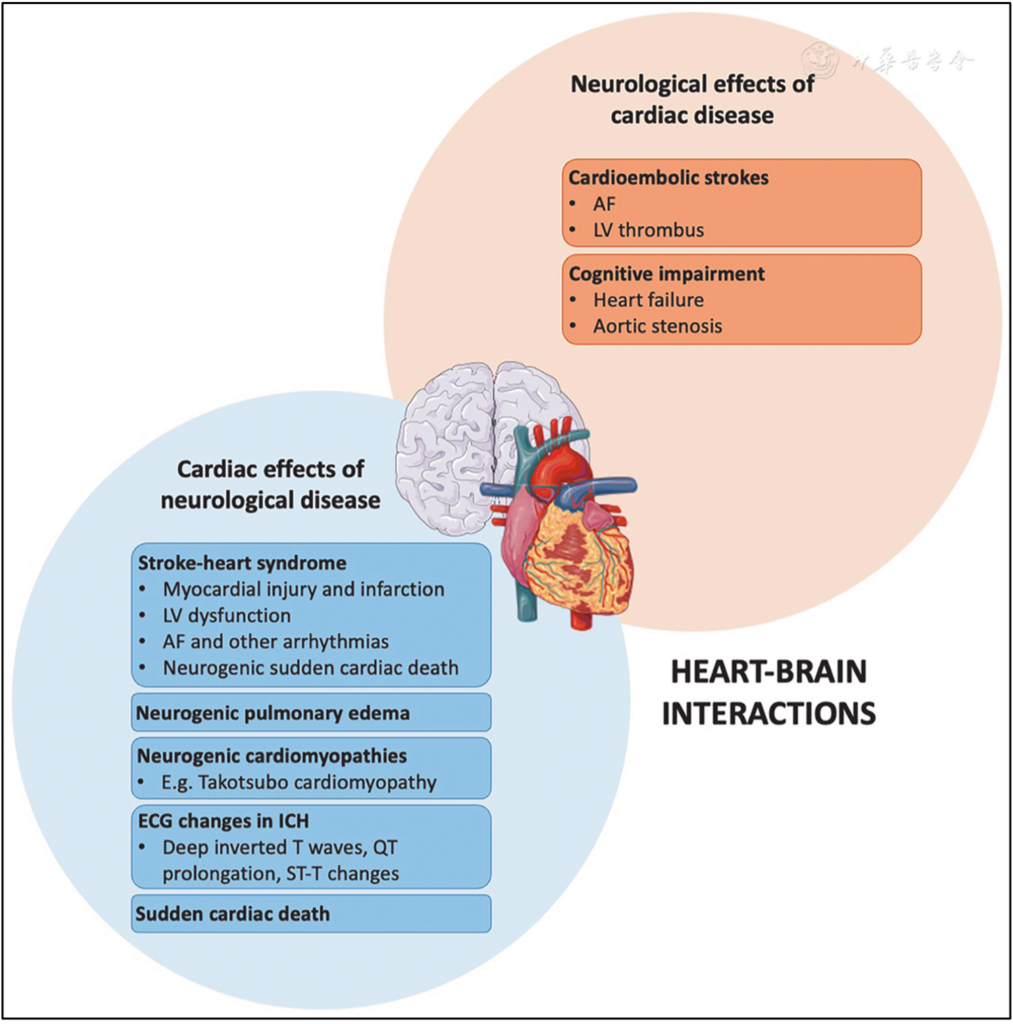
Image Source: Goh, F. Q., Tan, B. Y., Yeo, L. L., & Sia, C. H. (2025).
The Heart-Brain Axis: Key Concepts in Neurocardiology. Cardiology Discovery, 5(02), 162-177
(https://mednexus.org/doi/10.1097/CD9.0000000000000156)
Functional Brain Alterations in Cardiovascular Disease
In our systematic review of functional magnetic resonance imaging (fMRI) studies in cardiovascular diseases (CVDs)3, we found that cardiac dysfunction is frequently accompanied by altered brain activation patterns, particularly within the default mode, salience, and executive control networks. These disruptions were associated with impairments in attention, memory, and executive functions. Such neural alterations in brain network integration suggest that even in the absence of stroke, chronic cardiac conditions can precipitate subtle cerebral hypoperfusion and neuroplastic alterations, potentially accelerating towards cognitive decline and poorer task performance among patients with CVDs.
Vascular and Structural Correlates of Cognitive Risk
The relationship between carotid intima-media thickness (CIMT) and white matter hyperintensities (WMHs), as reviewed in another review paper4, further supports the vascular basis of cognitive impairment (CI). Increased CIMT, an early marker of atherosclerosis was consistently linked to higher WMH burden, reflecting microvascular damage and reduced cerebral perfusion. Significant factors influencing the CIMT–WMH relationship included age, hypertension, depression, migraine, Hispanic ethnicity, and apolipoprotein E (ɛ4) status in postmenopausal women. The study supported the association between carotid atherosclerosis (CAS) and WMHs, suggesting that vascular changes may drive white matter pathology. Overall, the findings reinforce the concept of the “vascular aging continuum”, where subclinical cardiovascular changes precede measurable cognitive deterioration5.
Neurohormonal Pathways and Emotional Health
Beyond vascular mechanisms, neurohormonal markers also bridge cardiac and neuropsychiatric domains. Our systematic review on NT-proBNP and depressive symptoms in cardiac patients6 demonstrated that elevated levels of this cardiac biomarker were predictive of depression prevalence or its increased severity. Approximately 31.3% of the cardiac patients exhibited depressive symptoms. In addition, depression was more prevalent among those with reduced ventricular function and NYHA class II–III functional limitations. The significant association between elevated NT-proBNP levels and depression suggests shared pathophysiological pathways, including systemic inflammation, autonomic dysregulation, and neuroendocrine imbalance. Such evidence positions NT-proBNP not merely as a cardiac risk indicator but also as a potential biomarker for brain-behaviour interactions.
Integrated Model of Heart–Brain Health
The clinical management of cardio-cerebrovascular diseases remains a major global public health challenge, given their shared risk factors, overlapping pathophysiology, and cumulative impact on morbidity and mortality7. Collectively, these studies illustrate a multidimensional heart–brain link that encompasses:
- Functional brain network alterations linked to cardiac dysfunction.
- Vascular structural changes connecting carotid pathology to cerebral white matter integrity.
- Biochemical biomarkers reflecting overlapping cardiometabolic and neuropsychiatric mechanisms.
These interconnected domains advocate for a systems biology approach to cardiovascular health, where prevention and rehabilitation extend beyond the myocardium to encompass cognitive and emotional well-being.
Future Directions
Future research should focus on longitudinal, multimodal imaging and biomarker studies to delineate causal pathways and reversibility potential. Integrating cardiac rehabilitation, neurocognitive screening, and psychological assessment into clinical protocols could offer a holistic framework for optimizing health outcomes. Moreover, interventions targeting both vascular health and neuroplasticity, such as exercise, cognitive training, and anti-inflammatory strategies may hold promise in mitigating the dual burden of CVDs and CI.
Conclusion
The evidence is clear: the heart and brain share a common destiny. CVDs are not merely a disorder of the heart; it is a systemic condition with profound neurological consequences. Recognizing and addressing the heart–brain continuum is essential for transforming clinical practice from organ-specific management to truly integrative cardiovascular–neurocognitive care in a real-time setting.
References
- Xu, S., Scott, K., Manshaii, F., & Chen, J. (2024). Heart-brain connection: How can heartbeats shape our minds?. Matter, 7(5), 1684-1687.
- Husain, M. (2025). Vascular health has an impact on brain health. Brain, 148(5), 1439-1440.
- Humayra, S., Yahya, N., Ning, C. J., Mir, I. A., Mohamed, A. L., & Manan, H. A. (2024). Brain functional alteration and cognitive performance in cardiovascular diseases: a systematic review of fMRI studies. Frontiers in Neurology, 15, 1425399.
- Humayra, S., Yahya, N., Ning, C. J., Raffali, M. A. A. F. B. M., Mir, I. A., Mohamed, A. L., & Manan, H. A. (2024). Relationship between carotid intima-media thickness and white matter hyperintensities in non-stroke adults: a systematic review. Frontiers in Neuroanatomy, 18, 1394766.
- Ungvari, A., Nyúl-Tóth, Á., Patai, R., Csik, B., Gulej, R., Nagy, D., … & Csiszar, A. (2025). Cerebromicrovascular senescence in vascular cognitive impairment: does accelerated microvascular aging accompany atherosclerosis?. GeroScience, 1-14.
- Humayra, S., Yahya, N., Ning, C. J., Mohd Raffali, M. A. A. F. B., Mir, I. A., Mohamed, A. L., & Abdul Manan, H. (2025). Clinical significance of NT-proBNP as a predictive biomarker of depressive symptoms in cardiac patients. Frontiers in Cardiovascular Medicine, 12, 1439520.
- Qi, C., Wang, W., Liu, Y., Hua, T., Yang, M., & Liu, Y. (2024). Heart-brain interactions: clinical evidence and mechanisms based on critical care medicine. Frontiers in Cardiovascular Medicine, 11, 1483482.
