What is Non alcoholic fatty liver disease (NAFLD)?
calgarygi.com
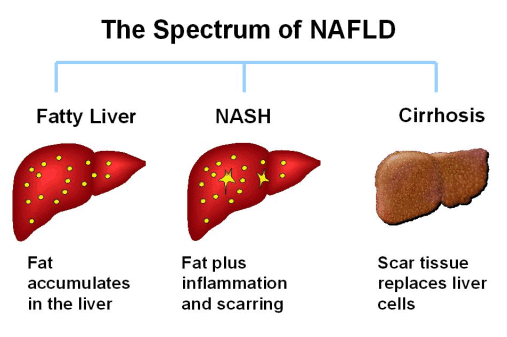
Non alcoholic fatty liver disease (NAFLD) is the accumulation of abnormal amounts of fat within the liver. NAFLD is classified as either fatty liver or steatohepatitis (NASH). In both of them there is an abnormal accumulation of fat in the liver cells, but, in addition, in NASH there is inflammation involving the liver, and, the liver cells are damaged, they die, and are replaced by scar tissue.
NAFLD has rapidly increased over the years and has become one of the most common causes of chronic liver disease in the western world and increasing in importance in other parts of the world. Understanding of the epidemiology and natural history of NAFLD has increased that the condition is not as “silent” as believed. Instead, NASH progresses to scarring and ultimately to cirrhosis, with all the complications of cirrhosis, for example, gastrointestinal bleeding, liver failure, and liver cancer. Approximately 30–40% of people with NAFLD develop NASH, and liver cirrhosis will develop in 40% of them with NASH.
Is NAFLD a common disease?

asianscientist.com
The prevalence of NAFLD in the general population of Western countries is 20-30%. The prevalence in our country remains unknown due to limited study. However, as a hepatologist in a government tertiary hospital, I have noticed the increasing number of patients with liver cirrhosis of “unknown” etiology nowadays (negative viral screening, autoimmune screening, and non alcoholic/drug induced). These patients have been labelled as “crytogenic” since long time ago! But if we look carefully the patients having metabolic syndrome among them, undoubtedly, I believe a significant number of them will have fatty liver disease. NAFLD is now recognized as the most common cause of cryptogenic cirrhosis.
Reviewing our local published articles, up to 22.7% of the “health screened” individuals were found NAFLD during a multi-ethnic health check-up population in Malaysia.1 Another study by Chan WK et al. had concluded that the overall prevalence of NAFLD among young Malaysian adults was found to be relatively low, however, the prevalence of NALFD was observed higher inordinately among Indian and Malay males consistent with the higher prevalence of obesity in these groups.2
What causes NAFLD?
NAFLD is part of metabolic syndrome. The International Diabetes Federation defines metabolic syndrome as the presence of central obesity based on ethnic specific cut-off for waist circumference, plus two or more of the following: raised triglycerides, reduced serum high-density lipoprotein (HDL) cholesterol, raised blood pressure and raised fasting plasma glucose. Insulin resistance and oxidative stress are believed as two major factors leading to the development of NASH.
However, not to be surprised that NAFLD can happen in persons who are lean, so-called ‘lean NAFLD’ which is described in Asian population initially.
Besides liver complications, there is now growing evidence that NAFLD is a multisystem disease, affecting extra-hepatic organs and regulatory pathways. NAFLD is associated with a significant risk of cardiovascular disease (CVD) and an increased morbidity and mortality associated with cardiovascular events.
What do I feel if I have NAFLD?
Most people with NAFLD live with fat in their liver asymptomatically. If you have NASH, you may have symptoms such as severe tiredness, weight loss, yellowing of the skin or eyes and skin itching. But it could take years for them to develop.

How to diagnose NAFLD?
The diagnosis of NAFLD is usually first suspected in an overweight or obese person who is found to have mildly elevated liver enzymes during a routine blood testing. The diagnosis can be confirmed with ultrasonography and following exclusion of significant alcohol intake and other causes such as viral hepatitis B and C. Fatty liver is recognized on ultrasonography based on the following features: increased echogenicity, posterior attenuation and loss of intra-hepatic architectural details. Currently, histopathological examination of a liver biopsy specimen is the only reliable way for evaluation of NAFLD.
If you have fat but no inflammation or tissue damage, we call it NAFLD.
If you have fat, inflammation, and liver damage, the diagnosis is NASH.
If you have scar tissue in the liver called fibrosis, it is cirrhosis.
How to treat NAFLD?
Unfortunately, there is no specific treatment for NAFLD. Lifestyle interventions are what you need:
- Losing weight
- Regular exercise
- Diet control (Mediterranean diet is more effective than a low fat diet)
- Lowering your cholesterol and triglycerides
- Controlling your diabetes
- Avoiding alcohol and unnecessary traditional medicine or over-the-counter (OTC) drugs
- In addition, bariatric surgery is also advised to patients who have morbid obesity.
Although lifestyle interventions have been shown to be effective, many patients find difficulty in following them.
Drinking coffee seems to decrease the risk of having fatty liver in some large cohort studies. Antioxidants such as Vitamin E, selenium and betaine may be beneficial and studies are underway. Ursodeoxycholic acid has been beneficial in some patients with elevated liver enzymes.
By Dr. Chieng Jin Yu, Medical Lecturer, Consultant Gastroenterologist and Hepatologist, Universiti Putra Malaysia (UPM).
[This article belongs to The Malaysian Medical Gazette. Any republication (online or offline) without written permission from The Malaysian Medical Gazette is prohibited.]
References:
- 1. Goh SC et al. Prevalence and risk factors of non-alcoholic fatty liver disease in a multiracial suburban Asian population in Malaysia. Hepatology International. 2013 Jun;7(2):548-54.
- Chan WK et al. Non-alcoholic fatty liver disease in a young multiracial Asian population: A worrying ethnic predilection in Malay and Indian males. Hepatology International, 8(1), 121-127.
