The causes of vomiting blood, or haemetemesis, are a myriad ranging from the most common to the least heard of possibilities. This article, however, concentrates on two issues that plague the community worldwide – bleeding peptic ulcer disease (PUD) and bleeding oesophageal varices (ruptured engorged blood vessels lining the swallowing tubes).
Some information about PUD and upper endoscopy (OGDS) can already be gathered from articles published on Malaysian Medical Gazette in the past (https://www.mmgazette.com/doc-whats-an-o-g-d-s-dr-chiam-keng-hoong/).
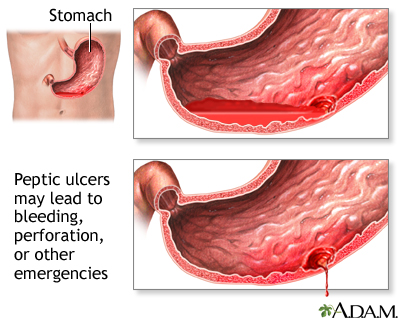 PUD increases the risk of hematemesis in the long run as does Helicobacter pylori infection, frequent ingestion of painkillers or traditional medications imbued with steroids. The above causes erosion of the protective lining of the stomach wall and reduces its natural protection from the acidic environment in the stomach. This can cause an ulcer to form which, depending on the severity, manifests as mild troubling tummy aches or causes the much feared complication of vomiting blood.
PUD increases the risk of hematemesis in the long run as does Helicobacter pylori infection, frequent ingestion of painkillers or traditional medications imbued with steroids. The above causes erosion of the protective lining of the stomach wall and reduces its natural protection from the acidic environment in the stomach. This can cause an ulcer to form which, depending on the severity, manifests as mild troubling tummy aches or causes the much feared complication of vomiting blood.
Another commonly encountered cause of haemetemesis is bleeding oesophageal varices. This almost always happens to patients who suffer from chronic liver disease, or liver cirrhosis. This is a condition where the liver architecture hardens from ongoing insult (hepatitis) and eventually forms extensive scarring. Such scarring is not good for the normally pliable liver tissue as it leads to an increase of pressure that builds up within the blood vessels feeding into the liver. Subsequently the elevated pressure is transmitted along these blood vessels and causes them to become engorged.
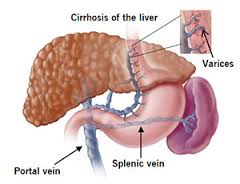 These engorged vessels can be visualised during an OGDS and they are usually seen around the linings of the oesophagus and the stomach. These two organs are in close proximity to the liver and branches of blood vessels feeding into them are also affected by the backlogged pressure. As the pressure escalates, so does the tendency of these swollen blood vessels to rupture. When they do, they lead to the typical presentation of vomiting blood.
These engorged vessels can be visualised during an OGDS and they are usually seen around the linings of the oesophagus and the stomach. These two organs are in close proximity to the liver and branches of blood vessels feeding into them are also affected by the backlogged pressure. As the pressure escalates, so does the tendency of these swollen blood vessels to rupture. When they do, they lead to the typical presentation of vomiting blood.
Patients with bleeding PUD or oesophageal varices often present in a sudden, abrupt/acute state which can be fatal if no medical treatment is carried out. Therefore upper gastrointestinal bleeding remains one of the most important topics all doctors need to be familiar with in order to provide adequate resuscitation before advanced management is carried out.
Patients and their next of kin should anticipate being triaged to the red zone upon presentation at the emergency department. Fluid, blood transfusion, specific pharmacological treatment and ongoing vital signs monitoring should be carried out.
A team of doctors specialising in acute medicine should attend to the patient and, upon stabilisation, will refer the patient to the attending surgeon or gastroenterologist for further management. Timing of OGDS depends on assessment scores for risk stratification which takes into account risks of rebleeding, co-morbidites and mortality.
Despite the advancement of therapeutic endoscopy during which bleeding can be stopped via different methods with great outcomes, many patients refuse this treatment option. Some cite the fear of swallowing a long tube while others fear pain arising from the procedure as it is usually performed with just minimal sedation.
There are, however, some patients who change their minds after a detailed explanation is given. This reminds us that basic concepts of OGDS and its benefits need to be explained to patients and their loved ones in order to eliminate the fear and stigma attached to the procedure. As a consultant once said to his patients, “Fear does nothing to solve the problem.” How true!
Dr. Chiam Keng Hoong is an internal medicine physician and a MRCP holder. He currently works in Sabah.
[This article belongs to The Malaysian Medical Gazette. Any republication (online or offline) without written permission from The Malaysian Medical Gazette is prohibited.]
