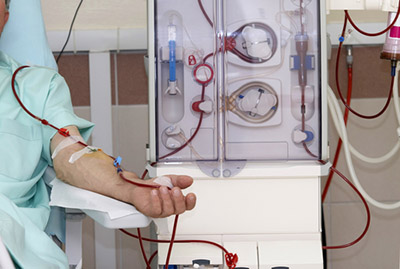
Haemodialysis
With increasing awareness regarding kidney disease and implementation of screening, more people are diagnosed with early chronic kidney disease. For many patients, the disease remains stable. Unfortunately for some, their condition worsens until symptoms of kidney failure emerge.
Patients with advanced disease are usually referred to doctors specializing in kidney disease, also known as nephrologists. They give advice and counseling to these patients in preparation for dialysis before complications occur. Nephrologists also educate patients with advanced kidney disease regarding the available dialysis choices and help them decide which option meets their health and lifestyle needs.
Many patients with advanced chronic kidney disease are only made aware of their condition once they develop life-threatening situations after their kidneys have failed. Upon admission to the hospital, an emergency dialysis catheter is inserted to allow temporary maintenance haemodialysis. Some patients are lucky enough to recover from the acute episode. However, most find themselves with permanently damaged kidneys and, once discharged, need to continue with long-term dialysis at a center near home. As they need to be on dialysis for the rest of their life, they need to have a permanent dialysis access.
In Malaysia, there are two dialysis choices available – haemodialysis and peritoneal dialysis.
Haemodialysis (HD) is done by removing blood from the body and pumping it through a blood filtering machine called a dialyser AKA an artificial kidney. The blood is channeled to the machine via a dialysis catheter or vascular access, for example an arteriovenous (AV) fistula or graft. The blood is filtered many times to remove waste and excess fluid. On completion, the filtered blood will be pumped back into the patient. HD needs to be done in a center with a dialysis machine, 3 times a week, for 4 hours each time.
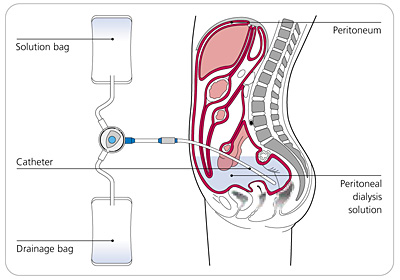
Peritoneal Dialysis
Peritoneal dialysis (PD) is a dialysis method that uses a patient’s own body to filter and remove waste and extra fluid. This is done by putting in dialysis solution, or dialysate, into the peritoneal cavity in the abdomen through a special catheter called PD catheter, which requires surgical insertion. The peritoneum, which is the membrane around the cavity, acts as a filter. The waste and excess fluid passes through the peritoneum and goes into the dialysate. After that, the dialysate is drained out and replaced. Changing the fluid takes about 30-40 minutes and usually needs to be replaced 4 times a day. PD can be done at home – either manually or automatically with the help of a machine. This can be done by the patient themselves or by a caretaker. Patients who opt for PD need to perform it daily.
Some people prefer peritoneal dialysis as no needles are required during the treatment. Many young patients with kidney failure choose PD as it can be done at home and while they are sleeping at night, leaving them free to work and take care of their families during the day.
However, there are also patients who prefer HD because they do not want to undergo the procedure of inserting a catheter, while others feel an AV fistula is more socially acceptable compared to having a tube protruding from the abdomen. Some patients choose HD because they have no dedicated carers available and are too frail or visually impaired to perform PD on their own.
Regardless of which mode of dialysis chosen, make sure you understand both pros and cons of the respective method. If you find it difficult to decide on a method which best suits your lifestyle, please talk to your doctor for further advice.
Dr Nur Hidayati is a permanent columnist for The Malaysian Medical Gazette and an internal medicine physician.
[This article belongs to The Malaysian Medical Gazette. Any republication (online or offline) without written permission from The Malaysian Medical Gazette is prohibited.]
